by Gregg A. Masters, MPH
Article discovered via the a ‘501 (c) 6 non-profit organization that allows Accountable Care Organizations (ACOs) to work together to increase quality of care, lower costs and improve the health of their communities’ . NAACOs et al weigh in on the Value in Health Care Act of 2020:
In association with the following health care industry advocacy groups including: the American Academy of Family Physicians, American College of Physicians, American Hospital Association, American Medical Association, America’s Essential Hospitals, America’s Physician Groups, the AMGA, Association of American Medical Colleges, the Federation of American Hospitals Health Care Transformation Task Force, Medical Group Management Association, National Association of ACOs and Premier have all endorsed the ‘Value In Health Care Act of 2020’.
The Act intends to:
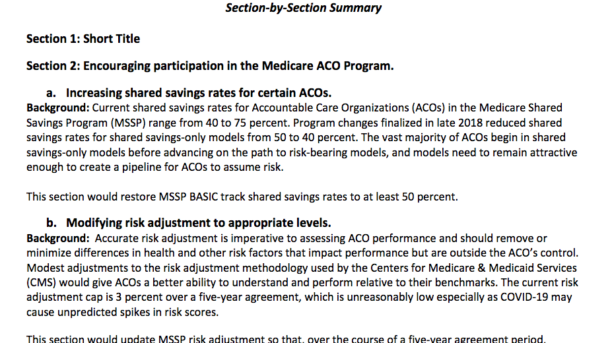
‘further strengthen ACOs and APMs and ensure their continued success. We are pleased that the bill provides appropriate shared savings rates, modifies risk adjustment methodologies, removes barriers to participation, ensures fair and accurate benchmarks, and provides educational and technical support for ACOs. The bill also makes important steps to reinforce the transition to value through extending and modifying Advanced APM bonuses and addressing aspects of APM overlap. These reforms will ensure that value-based care models continue to be viable for physician and hospital participants’
Read a section by section summary here.
Also, the American Hospital Association (AHA) further reports via a ‘Coalition Voices Support for the Value in Health Care Act of 2020‘.
In a letter to Representatives. Peter Welch, Suzan DelBene, and Darin LaHood, thirteen organizations representing health care providers, including the AHA, voiced support for the Value in Health Care Act, legislation to strengthen Medicare’s value-based payment models and accountable care organizations.
You can read the full text of the letter .
Clearly the systemic stressors associated with Covid-19’s impact on the usual and customary operations of U.S. healthcare financing and delivery may qualify as an unparalleled (perhaps ‘Black Swan’ scale) ‘may you live in interesting times’ challenge to healthcare leadership – perhaps of a lifetime?
So from a holistic perspective, it seems our leadership cohort across the continuum of an over-engineered, hierarchical, perhaps needlessly too complex but clearly stressed healthcare delivery and financing construct, we’re simultaneously presented with both clear and present ‘danger’ but also considerable ‘opportunity’ to re-engineer our change resistant healthcare borg?
If not now, when?
==##==